Billing is the lifeblood of any healthcare practice. For the most part, medical billing can be a very complicated and work-heavy procedure with many repetitive processes, but what about implementing an automated medical billing system?
Medical Billing Process
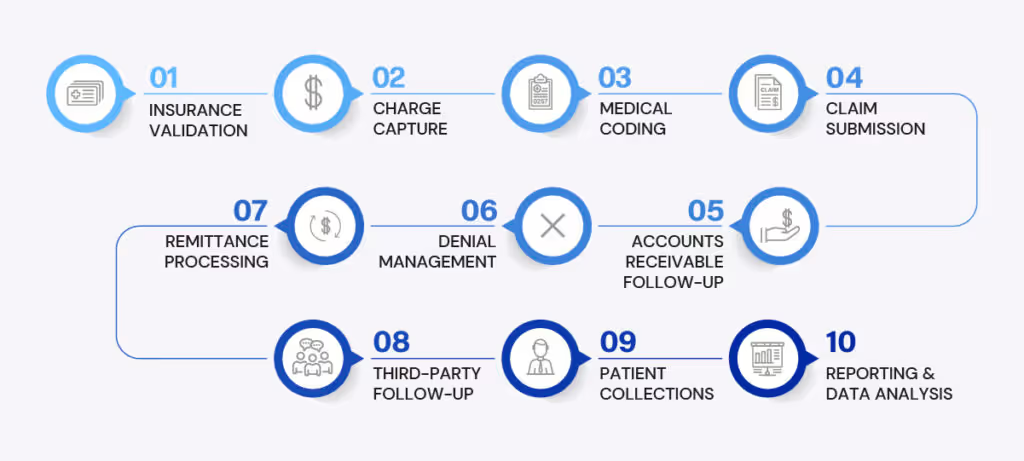
This repetitive nature of medical billing makes it a great candidate for automation and coupled with the fact that several organizations are under pressure to keep the medical billing process as efficient and reliable as possible.
In this article, we talk about automated billing systems in the medical industry, their importance, and the processes involved.
Why Does the Medical Billing System Need Automation?
Automation takes care of every important aspect of medical billing that might seem tedious to a human. Billing errors get identified before a claim is submitted, which results in claims getting paid faster by payers. Similarly, RPA payment solutions can enhance collections by automatically sending patient bill notifications through text or email.
In the United States alone, much money is being spent yearly on healthcare expenses that can be avoided. The following are some reasons why automated medical billing is critical.
Proper Documentation
In an industry where Paper document filings cost $20 per filing process. Healthcare providers fill out an average of 20,000 forms yearly. In medical billing, where lots of administrative paperwork like patient profile creation and registration, eligibility checks, and other billing information validation are being filled daily, error-free documentation should be the goal of every healthcare provider.
Similarly, automation enables providers to comply with HIPAA and other regulations and reduces the number of staff members dedicated to a process while increasing productivity.
Lower Costs
Take RCM, which is the financial process of collecting payments for medical bills to generate revenue for a healthcare organization. Revenue cycle management can be time-consuming and expensive because it combines administrative data such as a patient’s personal information, treatment codes, and the insurer’s name with financial billing information. The recommended amount of receivables older than 120 days should be between 12-25 percent, but automating RCM tasks aid in lowering it to less than 12 percent.
Streamlined Medical Billing
All healthcare providers that have jumped on the RPA train in Medical billing automation can attest that using an outdated billing system risks a high level of unorganized claims processes and unnecessary errors. In 2021, $28.91 billion in payment errors were made as a result of coding errors, according to the Centers for Medicare & Medicaid Services (CMS).
If you’re from the IT consulting industry, let us show how you can benefit from automation in consultancy for medical billing.
What Can Be Automated in Medical Billing?
A lot of tedious and repetitive processes can be automated in Medical billing. Let’s take a look at the most important ones.
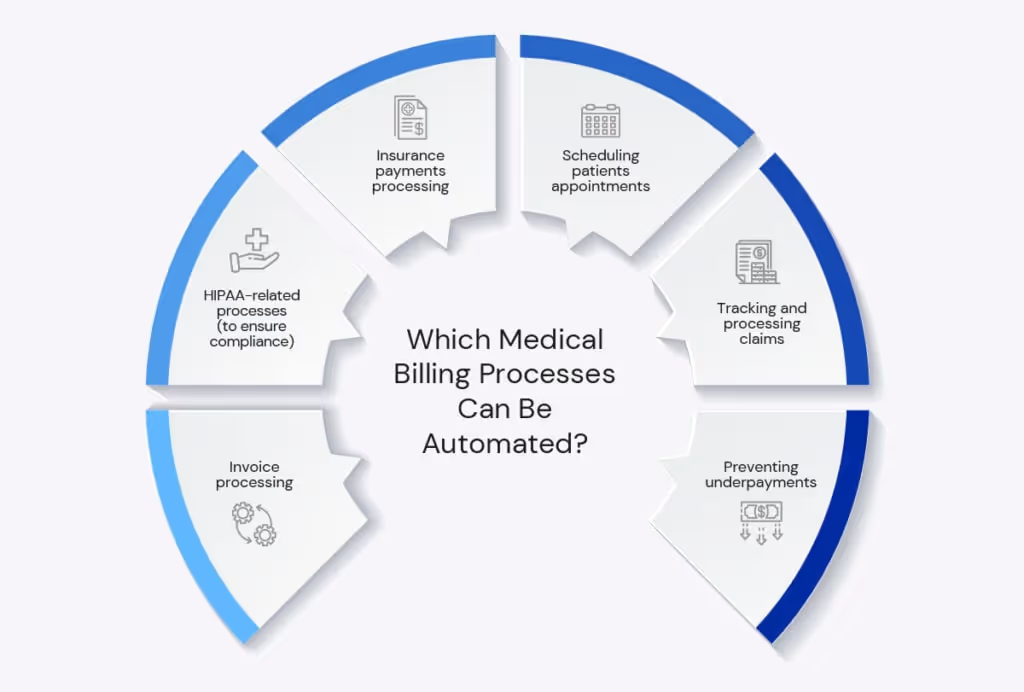
Appointments Scheduling
Automation can simplify patient scheduling processes wherein all appointments and registrations from the beginning up until the point of completion of a visit or consultation will be sorted by RPA bots.
Revenue Cycle Management
This is arguably the most important part of an automated medical billing process. Healthcare providers have to sort through disparate technology systems to source miscellaneous data such as entries from patients’ medical history, drug and disease codes, and insurance eligibility. Afterward, reimbursement is received based on the accuracy of medical billing codes. If the process isn’t implemented accurately, payments might not reflect.
HIPAA Compliance
To help remain HIPAA compliant and minimize security risks while facilitating a successful doctor-patient relationship, healthcare companies must embrace automation and integrate RPA within their system. Besides, penalties for HIPAA violations are quite severe, be it the healthcare providers’ fault or not.
Omissions and errors regarding document-related issues are not far-fetched because most of the procedures require filling in specific information approved by patients and usually involve chasing people down to get approvals. All these typically lead to skipping some systems and making the simplest errors. However, implementing RPA perfectly promotes automation in the healthcare workflow to help transfer patients’ data automatically.
Read more about HIPAA compliance automation.
Claims Processing
Claims processing automation like keeping fee schedules up-to-date, remittance, tracking claims, and posting of payments can ensure accurate prices so that no claim goes unpaid or underpaid. Leveraging RPA in claim processing can make your company clear of any loss you may incur due to underpayments.
Learn more about automated claims processing.
Electronic Health Records automation with RPA
Regardless of the type of Electronic Health Records software your company uses, there is always room for automation. Consider the following example:
Thinking of automating you medical billing management? Find out more here.
The Steps For Implementing Automated Billing System with RPA
Medical billing might seem a lot complicated, but it’s a process that comprises the following eight simple steps.

Registration
This is the first step of the medical billing process, where a patient calls to schedule an appointment with a healthcare provider. For a doctor’s visit, a patient has to pre-register effectively by providing insurance details. Information on old works will be saved, and a patient only has to explain the reason for their visit on subsequent visits. Registration enables medical billers the opportunity to verify details provided before claim submission.
Financial Responsibility Check
Financial responsibility checks are carried out to verify a patient’s insurance to know who owes what for a doctor’s visit. Before a biller can determine if a patient’s insurance plan covers the services the patient needs, the biller has to gather vital information that can only be carried out by carrying out financial responsibility checks.
Individuals and companies all have different insurance plans. Hence, a biller has to check a patient’s coverage to ensure certain bills are assigned appropriately and prescriptions are covered for the entirety of the bill. In this case, RPA bots carry out these kinds of checks.
Bookings
Patients are asked to fill out forms as they arrive to separate registered patients from first-timers. The necessary official identification, such as a valid insurance card along with a passport or driver’s license, is used in determining whether copayments are received before or after the enrollment is done by the providing office.
In most cases, Copayments are collected at the point of service, and once the patient has been verified, a report is sent to the medical coder. Upon receiving the medical news, the medical coder analyses it and translates its information into usable medical code. This medical coding process results in what’s called the “superbill.”
The superbill includes demographic information about the patient’s medical history, the physician’s name, the provider’s name, the codes for the diagnosis and procedure, the procedures performed, and other relevant medical information. The superbill is then transferred via a software program to the medical biller.
Coding and Billing Compliance Checks
After receiving the superbill, the medical biller transfers it into billing software or a paper claim form. It ensures that the procedures coded are billable, even though the billability of a system depends largely on the regulations laid out by the payer and the patient’s insurance plan.
Billers must also ensure that compliance standards are met. Typically the code must follow guidelines laid out by the Office of the Inspector General (OIG) compliance standards and the Health Insurance Portability and Accountability Act (HIPAA).
Transmitting Claims
Transmission of claims is done electronically and with coding through the use of EDI (Electronic Data Interchange). The Health Insurance Portability and Accountability Act of 1996 (HIPAA) mandates all health entities covered by HIPAA to submit their claims through electronic means. However, claims will only be transmitted through EDI if they are error-free. Learn how you can improve your claims management by providing RPA for claims processing.
Adjudication Process
This is the stage where a claim is denied, rejected, or accepted. A payer evaluates the medical claim to decide whether it is compliant or valid and how much will be reimbursed to the provider. During the adjudication process, the details of the claims are sent to the biller or provider to know how much they are willing to pay and why.
For patients with secondary insurance, the remainder of the claim is sent to their secondary insurer after approval by the primary insurer. An appeal process can be filled with the payer if any problem arises.
Generate Patient Statements
Patient statements detail all the patient’s care from their healthcare provider. It is the procedure bill, and once the payer sorts the agreed amount, the patient handles the rest. Some payers might include an Explanation of Benefits (EOB) to explain why some procedures were covered and others were not.
Follow Up On Patient Payments
Bills must be paid on time to ensure a system functions without issues. Billers are charged with mailing out timely, accurate medical bills to ensure bills get paid on time. Each provider has its own set of guidelines and timelines when it comes to bill payments, notifications, and collections. The biller’s responsible for ensuring that the provider is properly reimbursed for their services if the patient does not pay the full amount or is delinquent in their payment.
Learn more about five processes for the healthcare industry you didn’t know could be automated.
Automated Medical Billing – Conclusion
A streamlined and optimized workflow allows for a less hectic work experience. An automated billing system helps healthcare providers reduce human-related mistakes and accurately process claims.
Using Flobotics automation services, our in-house RPA developers (including UiPath consultants) are ready to help optimize your medical billing process by syncing multiple health data with your company’s database. Get in touch with us to get RPA consulting services now!
Like the article? Spread the word









.png)




