Insurance Claims Processing Automation With RPA: Reasons for Implementation and Use Cases
The insurance industry is notoriously bad at serving customers. But not in China. In the past few years, Chinese tech giants have made tremendous strides to become insurance innovation hubs. Take a look at just one example: WeSure, an insurance platform powered by the WeChat messaging app, celebrated its second anniversary with over 55 million users. This means that the biggest challenge for Chinese insurers today is not just to digitize businesses but to go beyond traditional offerings and even combine insurance with other financial services. To compete, insurance companies are revolutionizing the industry using Robotic Process Automation.
The Customer Satisfaction Score (CSAT) and Net Promoter Score (NPS) are the most important metrics for any insurance company. However, they lag far behind in the US as insurers fall short of expectations due to growth in other industries. Since the grievance process greatly impacts customer satisfaction, let’s look at how RPA insurance bots can revolutionize costs, operations, and customer experience.
Robotic Process Automation in Insurance
Robotics Process Automation, or RPA – using desktop-level front-end software bots that do not require programming to handle routine processes at the keystroke level – is revolutionizing insurance. From underwriting and onboarding personal and commercial insurance companies to serving insurers and handling claims, RPA is already revolutionizing how insurers work, improving customer service and reducing cycle times while cutting overhead costs.
Are you faced with reducing and minimizing the time for processing insurance documents? Find out how to accelerate these efforts here: How To Process Over Half a Million Insurance Documents In 8 Weeks.
RPA is also the fastest-growing technology in the field to date, with current trends showing that the RPA market, valued at $ 199.1 million in 2016, will grow at a compound annual growth rate (CAGR) of 60.5% through 2024. As per P&S Market Research, the global Robotic Process Automation market will reach unimaginable heights. Simultaneously, it is predicted that the demand for software robots in the field of intellectual work will continue to grow.
RPA affects all industries: new jobs will be created as large-scale RPA software is introduced. Companies will need to find the right balance between robotics and up-skilling existing employees.
Nevertheless, what about the insurance industry in particular?
In insurance, RPA is defined as the implementation of software robots that can be configured for each computer without the need for code. These software robots help their real-life technicians perform monotonous and repetitive insurance routines such as data entry.
In insurance operations, RPA effectively engages a workforce with artificial intelligence (AI), that is, robotic assistants who can execute basic computer commands of employees, performing various low-value-added tasks that currently consume these employees’ efforts, energy, and moral spirit.
Insurance robots work similarly to Excel macros. But unlike Excel macros (which only work in Excel), RPA insurance bots can run on multiple systems rather than being limited to one. Thus, these robots can work at the level of individual data fields in all insurance systems.
RPA platforms like UiPath, and Blue Prism can handle actions down to the mouse and keyboard levels. Once set up properly (more on that in a minute), they can do everything from opening apps to tapping, copying, and pasting information from one app to another, sending emails, and more.
For established insurance companies, operations have traditionally (and largely) relied on outdated legacy systems (with complex moving parts) that do not interact well with each other. This has led to the need for highly paid IT professionals to bridge these disparate systems effectively – which amounts to grueling days spent decrypting and arranging data:
- opening emails,
- copying and pasting data between legacy systems,
- creating PDF files,
- etc.
Thus, the Tower of Babel problem — the inability of legacy systems to “talk to each other” without manual human intervention at the keystroke level — created an insurmountable obstacle to optimizing existing technologies without a wholesale (and costly) rethinking of the company’s entire IT infrastructure. So it never happened.
The bar is lower for new insurance companies. They face fewer difficulties given their ability to use primarily cloud infrastructure from the get-go. Compare their situation to that of well-established insurance companies, and you will see that it is costly to invent basic systems that usually fall short of the automation promises.
This is why insurance companies – perhaps especially the big ones – are so excited about RPA. Finally, it allows them to use robotics in the insurance industry to “bridge the last mile” of their legacy insurance systems in ways that improve customer service and back-office efficiency.
Unsurprisingly, RPA is changing the way insurance companies do business.
As you probably know, insurance operations require complex processes and system connections to run a business, including underwriting, claims management, and risk analysis.
Nonetheless, insurance companies using RPA can make these processes more efficient – sometimes a staggering 50 percent – by reducing the cumbersome and time-consuming data entry and transcription tasks in legacy systems.
Reasons for Implementing RPA in the Insurance Industry
Insurance companies face many challenges:
- Customer expectations for lead times and multi-channel access continue to rise
- Intensive operations such as claim processing continue to hinder profitability.
- Complaints handling includes several management, administrative and customer service functions that manually perform resource-intensive tasks to protect the company from fraud or error.
Despite all this, in the US alone, the insurance industry loses $ 80 billion annually due to fraud (Coalition Against Insurance Fraud). It’s no surprise that RPA claims processing is emerging as a new trend in the insurance industry.
Because the company’s service standards and customer commitment are at stake, there is little room for error, and the cost of accurate claims handling should not be underestimated. This is why more and more companies are turning to robotic process automation (RPA) to solve these problems.
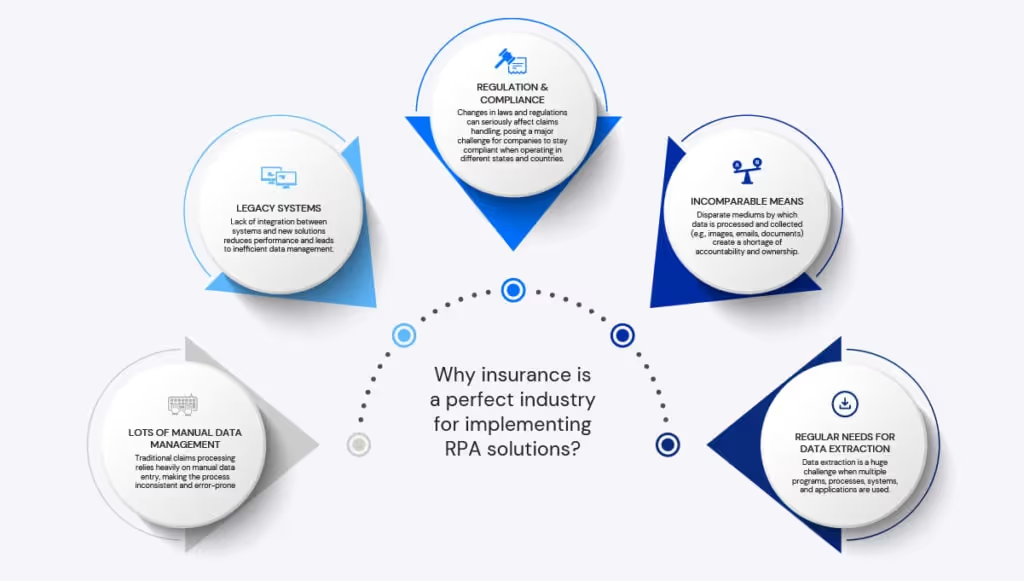
Some of the challenges associated with handling claims efficiently and error-free include:
- Manual data entry: Traditional claims processing relies heavily on manual data entry, making the process inconsistent and error-prone.
- Incomparable means: Disparate mediums by which information is processed and collected (e.g., images, emails, documents) create a shortage of accountability and ownership.
- Legacy systems: Lack of integration of these systems with new solutions reduces performance.
- Data Extraction: Data extraction is a huge challenge when multiple programs, processes, systems, and applications are used.
- Regulation and Compliance: Changes in laws and regulations can seriously affect claims handling, posing a major challenge for companies to stay compliant when operating in different states and countries.
These challenges impede insurance companies’ efforts to improve operational efficiency, reduce costs and improve customer service.
The decision to automate insurance duties can help here.
Claims handling with RPA ensures error-free tasks, simplifies data entry, and streamlines processes, resulting in lower operating costs, faster processing times, and greater compliance.
The productive impact of insurance claims processing automation is manifested in many aspects. We present and briefly discuss 10 of the most important ones.
Top 10 benefits of using RPA in the insurance industry
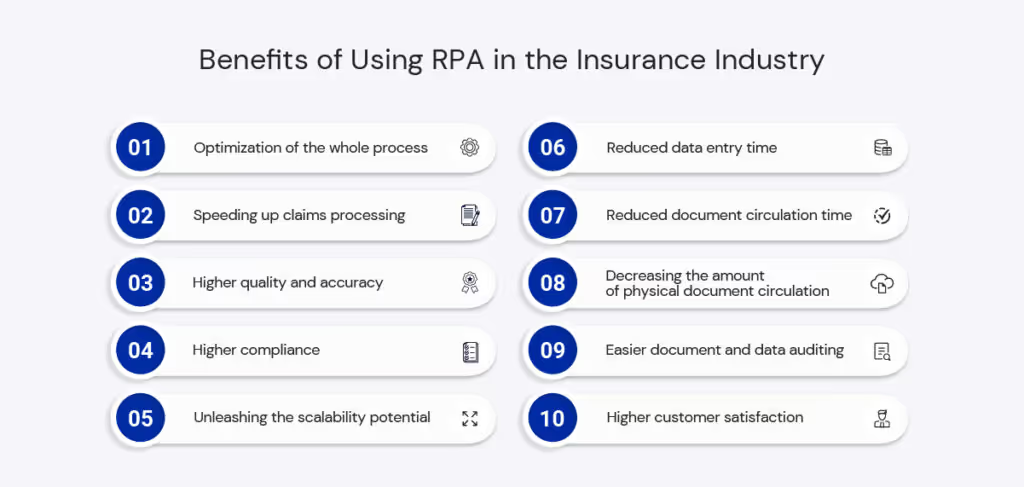
1 – Optimization of the whole process
RPA helps insurers simplify claims processing by streamlining multiple processes, including entering data into the system from various channels such as email, telephone, or online forms, checking coverage, and issuing settlement notices. A claims proofreader bot like the IQ Bot can eliminate the tedious manual processes of reviewing policy claims and checking for fraud. A bot can speed up processes – from organizing data, retrieving to transferring – without human intervention.
2 – Speed up claims processing
Following the previous point, an automated bot allows employees to focus better on interacting with customers than dragging and dropping documents from one department to another. This improves efficiency by structuring the vast amounts of claims data flowing through the department and increasing customer satisfaction by speeding up the claims handling process. This frees the claims processor from manual validation and data execution to focus on other steps that require human intervention to make decisions. Read more about how we can help you with claims processing automation and the benefits.
3 – Higher quality and accuracy
RPA not only reduces the backlog but also reduces the inevitable human error. For example, property and accident insurers need to assess damage estimates accurately. But since this information comes from various paper or PDF forms, it cannot be easy to maintain perfect accuracy whenever done manually. Having a bot to manage repetitive tasks such as data entry, validation, and cross-validation of coverage requirements can lead to a fast, efficient, and accurate claims process. In case of inaccuracies or deviations, the bot may require human intervention for further investigation.
4 – Higher compliance
Insurance companies are strictly regulated and must comply with laws set by various local and global regulatory bodies. Enforce these rules more closely by letting the bot document each step of the claim processing. This will dramatically improve insurance compliance and governance as companies can track and validate records continuously without depressing about errors or missing data.
5 – Scalability
One of the biggest pros of RPA is the creation of a virtual digital workforce that can be easily scaled up or down based on seasonality. With increased workload during peak periods, RPA can be a lifesaver for those handling claims. These bots ensure that work continues without delays and policyholders are not hurt by the spike in claims processing while still being 100% accurate.
6 – Reduced data entry
Clients are required to complete numerous forms as part of the claims handling process. The information obtained from these forms must be entered into a centralized system. Processing is not possible if this information is not available in electronic format.
Before automation was widely adopted in the claims industry, entering this data into the system was manual, time-consuming, and costly. However, modern technology has allowed software to directly read information from forms and enter it into the system. Consequently, converting data from paper forms to electronic records can be done with minimal manual intervention.
Since data handling is one of the biggest costs incurred by any insurance company, reducing the volume of data entry goes a long way toward saving costs.
7 – Completeness of the application
The lack of complete data is a serious obstacle to the fast processing of insurance claims. The reality is that different types of documents must be provided to obtain insurance. The list of these documents varies from case to case. Therefore, creating a simple checklist that can be verified is impossible.
Because the requirements are complex, most insurance consumers miss the opportunity to provide certain information from the outset. Consequently, their application is sent back, and they are asked to provide additional documents. The process is usually repeated several times before the claim is processed.
The repetitive nature of this process is a problem for insurance companies and consumers. This is because consumers must wait longer before receiving their money. From the insurer’s perspective, the continuous back-and-forth movement means that the efficiency of the back office, as well as the front office staff, decreases, leading to increased costs.
8 – Eliminates the need for storage
As mentioned above, the claims handling process requires a lot of paperwork. Insurance companies must keep these documents for future reference. This becomes a problem because it is tough to maintain a physical archive.
With the growth of automation in the claims processing industry, physical archives are outdated. Now they are being replaced by electronic archives. Electronic archives are easier to maintain. This is because the archiving process, as well as the receipt of documents, can be automated. This means that significantly fewer people and money must be spent on maintaining the archive. In addition, since the electronic archive does not take up much space in the real world, real estate costs are also saved.
9 – Audit log
The best thing about automating the complaints-handling process is that auditing becomes extremely simple. Suppose any insurance company manager has access to a specific file of the claim or performed any action related to the claim. In that case, this information is automatically recorded by the system. This way, the software creates a footprint that can be easily verified during an audit. This feature is essential for insurance companies that have lost funds in the past due to the connivance of their service personnel by outsiders.
10 – Visibility to the client
The entire claims handling process is a black box from a consumer perspective. This means the consumer does not know what is happening with their application until he receives the money. This creates a sense of ambiguity and uncertainty. Consumers do not mind waiting a little longer while they know what is happening with their requirements.
New and modern software for the automated processing of claims allows the timely provision of this information to customers. Clients are often presented with a flowchart explaining the different stages that their claim must go through. The dashboard provides customers with real-time updates when they log in. Thus, automated claims handling software not only lowers costs but also improves customer service.
Bonus benefit – Identifying fraudulent claims
Automated claims processing software can also detect patterns in data. Hence, whenever auditors discover a fraudulent claim, they must flag it in the system. Over time, the program developed its database of fraudulent claims. The system can then perform analytic operations on that data to uncover patterns typical of these fraudulent claims. The software can then use this information to flag new claims that follow the same way and, therefore, may be fraudulent. Most claims processing programs can learn continuously as more and more data points are attached to their database over an extended period.
Real-life use cases from the market
The insurance industry’s robotic automation use case is defined as documenting a list of insurance transactions/steps performed at the employee level. These actions and measures, performed on computers or other electronic devices, are then used to automate the movement of information in insurance applications.
IT consultants or your staff uses the insurance RPA use cases as drafts to implement automated scenarios that run across multiple systems to process data.
To help you learn, appreciate, and draw inspiration from how the insurance industry is deploying RPA, here are six examples of how insurance companies are adopting the technology in the United States, Europe, and Asia.
Also, see 40 Real World Use Cases of Robotic Process Automation Across Industries.
Use Case 1: Prudential Financial
Goal: Achieve precision, efficiency, and cost control
Company info:
- The company is headquartered in Newark, New Jersey.
- In business for almost 145 years
- Services to institutional and individual clients from over 40 countries
- The 2017 annual report shows the total revenue is $ 53.6 billion.
Prudential’s VP of Robotics Process Automation, Anne Delmedico, leads the Robotics Process Automation Center of Excellence. In September 2017, she presented how her company deployed a global RPA solution.
RPA was part of a larger, corporate-wide “transformation program” to drive strategic growth, improve customer service, and manage costs. Prudential picked Blue Prism as its RPA software solution.
Delmedico highlighted in her keynote that the company approached its decision to implement RPA with a value proposition rather than industry trends. The insurer intended to reach three main goals:
- accuracy,
- efficiency,
- cost management.
The first application of RPA at Prudential was to help handle payment discrepancies. Potential solutions were identified using automation to determine if there were two policies for the same person, look for the inversion of the policy number, and check if the policy was loaned. The company will contact the bank if no positive matches can be found in these categories.
Result: The infrastructure to start the process was created in July 2016; the first implementation was rolled out in October – just three months later!
By the end of 2016, Delmedico notified that ten automation processes were in production, resulting in savings of $ 500,000.
Use Case 2: Safe-Guard
Goal: Faster document processing, higher customer satisfaction scores
Company info:
- Based in Atlanta, Georgia.
- In business for 25 years
- Handles nearly four million contracts a year
- Serves over 11 million consumers
Safe-Guard offers products and solutions for the automotive industry and partners with Ford, Harley-Davidson, and BMW.
Irvine, California-based Kofax, a global RPA software provider, has published a case study describing how it helped Safe-Guard move from paper-intensive claims processing to a more efficient and automated process. According to Tim Dewey, former Safe-Guard VP of Operations Technology:
“We sell many financial and insurance products through car dealerships, which typically rely on pen and paper. Claims processing was an equally time-consuming process. In each of these areas, we need to collect significant documentation from external stakeholders and clients. Our administration teams have spent much time and effort scanning and processing paper documents and viewing and sorting email attachments into folders.”
Using the Kofax suite of products, the company has implemented several automated solutions. One of the first steps was to automate the process of drawing up a contract and filing claims. Paper documents are primarily scanned and uploaded to a centralized portal. After that, documents can be received by mail, email, or fax. They are identified by document type and then sent to the work queue for further processing.
An automated document extraction process then extracts the categories of information that Safe-Guard deems relevant and stores it in the system. Each step is monitored and analyzed to identify high-performance points and opportunities for improvement.
Result: As a consequence, Kofax reports that document processing time has been reduced from two hours to 10-15 minutes. Processing of documents has been reduced from five times to one, that is, by about 80 percent. Overall productivity increased by 30 percent, resulting in a 15 percent increase in customer satisfaction.
Use Case 3: Farmers Insurance Group
Goal: Increased satisfaction of both agents and customers
Company info:
- In business for over nine decades
- Serves over 10 million households
- Processes over 19 million individual policies
- It covers all 50 states
Farmers Insurance, based in Woodland Hills, California, prepares policies for vehicles, homes, and small businesses. Besides, it offers a wide range of other insurance and financial services.
Evidence of farmers’ RPA efforts can be seen in a case study published by Pegasystems. Pegasystems (“Pega”), founded in 1983 and based in Cambridge, Massachusetts, develops software for operational solutions and customer interaction solutions.
Farmers partnered with Pega to develop an automated software solution to provide agents serving small business customers with real-time support and a more intuitive interface. The goal was to enhance the agents’ ability to respond to Famers’ small business customers’ unique needs.
A year after the rollout, Pega says its business process management (BPM) technology has enabled the insurance company to double its market share. However, the exact number was not specified in the study.
Main results:
- The time it takes to form quotes has been reduced from 14 days to 14 minutes.
- Umbrella policy sales were up 70 percent.
- The new policy system was rolled out in less than five months.
- The satisfaction of agents and customers has increased.
Additional results: Other efficiency and time-saving tools built into the automation protocol, such as the ability to pre-fill applications for agents serving new customers, are discussed by Mhais Samalya, President of Commercial Business Insurance, in the 3-minute video (in the top right corner of the page).
In June 2018, additional evidence of RPA adoption at Farmers was cited in a Wall Street Journal article about the company. According to this feature, RPA is being used in a pilot program specifically to “automate a complex and routine process for claims adjusters.” Rehan Ashroff, director of the innovation lab and new ventures at Farmers Insurance, explains that the pilot aims to reduce turnaround times, improve efficiency, and shorten the payout period from weeks to days – or hours.
Use Case 4: New York Life
Goal: Automation at the hands of business administrators, not IT professionals
Company info:
- Almost 175 years in business
- Strengths in Mutual and Life Insurance
- National and Global
- Operating income of $ 2.06 billion, according to the 2017 annual report.
- Its 2017 operating profit was the largest in the insurer’s history to date
When New York Life realized it was handling over a million back-office transactions a year, it was looking for smarter ways to improve its processes and increase efficiency. So New York Life dealt with Pega to develop an automated back-office application called Processflow.
With Process flow, business administrators can quickly change processes, change steps, or reorder steps. In this three-minute video, Miguel Suarez, VP of New York Life Direct, and Jason O’Brien, TBC, New York Life Direct, give a presentation discussing the case study.
Result: At the time of the presentation, 84 of the 128 tasks in this workflow were either renewed or added to the system by a business administrator, not an IT professional.
Use Case 5: Zurich Insurance
Goal: Save effort, speed up processes
Company info:
- Almost 150 years in business
- Serves over 210 countries
- The 2017 annual report shows the total revenue is $ 64 billion.
- Investment portfolio $ 207 billion
- According to the Insurance Information Institute, it is ranked fourth among the top 10 commercial auto insurance authors in terms of direct premiums in 2016.
Zurich Insurance, a global diversified insurance company based in Switzerland, offers products and services for property, casualty, and life insurance. It is also the parent company of the Farmers Insurance Group.
The company reportedly decided to implement RPA by hiring London-based RPA software developer Blue Prism. In September 2017, Blue Prism published a case study describing how it helped a global insurer improve the management of international insurance contracts.
Before RPA, the execution and closure of international contracts in Zurich required a significant investment of staff time – particularly, four to five hours of transaction time per policy – and more than 1000 steps and substages from start to finish. Property and liability insurance are particularly ripe for RPA adoption due to their high volume and overlap with other lines of business.
Zurich was planning an initial deployment of the automation process in five countries, including the UK and Germany. At the time of the case study, Blue Prism robots were produced in these two countries.
Results: The results are remarkable. RPA implementation has lessened policy transaction times from nearly five hours to 40 minutes to 1.5 hours. In addition, Blue Prism claims that “exceptional” processes reduced effort by 20 to 30 percent, while straight-through processing reduced the effort required by 70 percent.
Use Case 6: Aegon Life Insurance
Goal: Automation of 120 basic tasks
Company info:
- Founded in 2007
- Headquarters in Mumbai, India
- Serves an international clientele with tools for asset management, life insurance, and retirement benefits.
A case study posted by Pega illustrates how Aegon Life Insurance implemented RPA.
The insurer first identified opportunities to improve customer service management. For instance, manual legacy business processes often required “multiple steps to validate information regarding user IDs, compliance, policies, and checklist requirements, according to the case study.
These time-consuming tasks were mature goals for moving to an automated framework. At the time of this writing, Pega worked with Aegon to manage and automate approximately 120 core business tasks.
Reported results:
- Expedited Claims Resolution – processing time reduced by 60 percent
- A 20% increase in the Net Promoter Score (NPS), an important metric of customer and employee satisfaction
- Total savings 84%
By using RPA, Aegon has saved time previously spent on staff training or manual completion of tasks. The time savings also contributed to better customer service.
The insurer’s contact center increased the first call resolution rate from 50 percent to 80 percent.
Conclusion
Insurers continue to face challenges with rapidly changing customer needs and heightened competition. As the insurance industry relies heavily on efficient back-office processes, insurers have begun implementing RPA to automate transactional, routine, rule-based operations so capital and talent can be repurposed to address more complex and strategic challenges. Robotic process automation is used to promote long-term success and productive market opportunities.
RPA in insurance can help achieve higher margins, greater compliance, sustainable company growth, and superior customer service while lowering costs and minimizing customer abandonment. Repeating the versatility and advantages that automation can bring, its adoption in the insurance sector is expected to be inevitable.
We at Flobotics, with our UiPath developers, provide end-to-end RPA solutions tailored to your organization. We use RPA as a deeper strategic tool to help you get the most out of it. From assessing the feasibility of a business unit proposal and developing a scalable program to implementing a solution across your business, we do our best for you. We fully back you in analyzing the best automation capabilities that deliver fast results and take your business to the next level.
Choose the right people to take advantage of RPA’s vast insurance benefits. Drop us a note via this link, and we will answer soon.









.png)




