Picture a standard medical procedure. You visit your primary care physician for the initial diagnosis. They prescribe a medication or refer you to another specialist. Some cases may require lab tests, long-term treatment, or hospitalization. All key details are saved in your patient history once the treatment is complete, covered, and paid for.
Behind the scenes, this rudimentary procedure involves moving heaps of medical records between healthcare providers, facilities, labs, pharmacies, and insurers. Typically, all of them use their internal systems to store patient data, so for all this process to function with minimum error and delays, healthcare organizations need one crucial ingredient: interoperability.
But what is interoperability in healthcare, really? What software systems are involved, which regulations and standards apply, and—crucial from the RPA perspective—how can automation support healthcare organizations in connecting seamlessly? Let’s find out.
What is Interoperability in Healthcare?
In healthcare, interoperability means the ability of multiple software systems (such as Electronic Health Record software—EHR, Hospital Management Systems, Medical Billing Software, etc.) to exchange and use medical data. An interoperable medical records network allows all entities involved in the patient’s journey to retrieve and view consistent medical records at multiple locations simultaneously.
As a result, providers can easily go through historical patient data to better understand each case and achieve the most optimal outcomes based on data. And patients don’t need to worry about forwarding or carrying around their documentation, insurance coverage, or lab results, regardless of where or which provider they need to consult. Seems excellent, right?
Healthcare Interoperability Levels
The Healthcare Information and Management Systems Society (HIMSS) distinguishes four healthcare interoperability levels that describe how interconnected a system is.
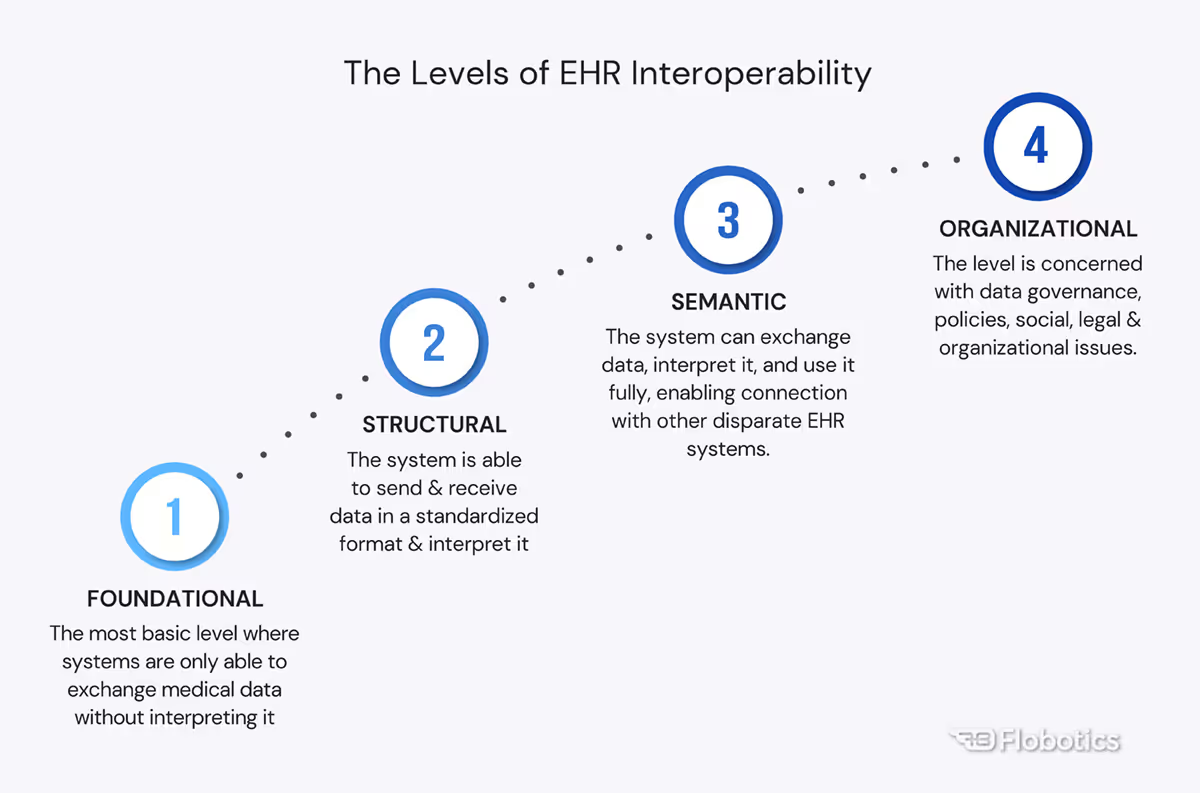
Challenges with Ensuring Healthcare Interoperability
One thing to note here is that true interoperability in EHR and other healthcare systems involves the transfer, interpretation, use, and governance of medical data. The transmitted data must be standardized to allow it so that all systems can understand it.
However, connecting dozens of disparate EHR systems can be a challenge. This is largely due to differences in terminology used by different providers, EHR functions, or technical specifications, and disparate data structure, which may lead to duplicate or faulty records, missing information, and, as a result, substandard and delayed services.
Another important hurdle comes from cultural differences. Some healthcare providers may share incomplete records and use siloed or fragmented data. In the most extreme cases, providers may deliberately block or limit the flow of patient records to increase their revenue and market position.
To make matters even more complicated, there’s the sheer variety of data. Patient history, personal data, treatment plans, doctor’s notes, test results, prescriptions, imaging, and diagnostic reports must all be kept in formats that enable easy sharing and access for all involved parties, from physicians to insurers.
Why is Interoperability Important?
Healthcare delivery is a team effort where all involved entities work toward a positive patient outcome. This is only possible if all roles can communicate and exchange information efficiently, meaning that interoperability in healthcare is paramount to their success.
Through the past decade, providers have made significant progress in transitioning from physical data storage to easier-to-share EHRs and other systems. As of 2021, 78% of office-based physicians in the USA and nearly all non-federal acute care hospitals (96%) adopted a certified EHR. Europe follows this trend, with increasing numbers of healthcare providers, hospitals, and practices deploying software systems to streamline their services.
This is a step in a good direction, as interoperability in EHR aims to ensure that all providers can exchange and use patient records. Aside from improved cooperation, it has a far-reaching positive impact on multiple aspects of healthcare operations:
- Higher productivity and revenue — EHR interoperability allows all involved entities to do more faster by improving data access. Instead of spending their time retrieving patient data, physicians can accept more patients.
- Data safety and compliance — A well-synergized and regulation-compliant data-sharing system is the best way to prevent leaks during patient data transfer.
- Lower costs — Better data operations translate into savings: fewer non-compliance fees, no-shows, and negative payment adjustments, combined with optimized patient transfers, improved analytics, and faster payments.
- Reduced physician burnout — On average, physicians spend 4.5 hours each day working with EHRs. Interoperability helps prevent physician burnout by reducing paperwork, manual data entry, and the time needed to retrieve the necessary records.
- Improved quality of care — With complete access to all medical details of each patient, physicians can diagnose the problem with better accuracy and suggest tailored, targeted treatment. On an organizational level, providers can use data to monitor care quality and identify improvement opportunities.
- Patient education — By connecting EHR systems with patient portals, physicians can communicate directly with patients to update them on test results, give recommendations, or suggest further care.
What Systems Can Be Interconnected?
Interoperability requires synergizing a range of systems involved in healthcare. What are they?
Electronic Health Records (EHRs)
Coordinating Electronic Health Records systems is essential for providing efficient patient healthcare services. This is especially true for those with complicated health issues who require the assistance of multiple providers. Interoperability reduces the time needed to retrieve records and eliminates the time-consuming process of unifying siloed data from various entities. Seamless access to EHR data from all sources helps providers streamline diagnostics and ensure timely and high-quality treatment.
To ensure the interoperability of two or more EHRs, all must be able to communicate, retrieve, and interpret patient data. There are several technologies they can use for that.

Medical Devices
Clinicians can leverage the network connection capabilities of modern medical devices to reduce manual record-keeping tasks. Instead of manually copying the relevant information, physicians can pull it directly from these connected devices in near real-time, enhancing care quality, safety, and efficiency.
For instance, connected medical devices like telemetry monitors or ventilators could alert physicians of an urgent patient condition. Connected equipment can also handle routine patient check-ups, saving hospital staff daily hours.
Health Information Exchanges (HIEs)
Health information exchange (HIE) is the ability to transfer healthcare data among medical facilities. This exchange can occur on patient portals, mobile apps, and other devices. The term can also refer to organizations overseeing the standards governing the exchange of health records.
By enabling healthcare systems to communicate with one another, HIEs play a crucial role in developing interoperability in EHR systems. However, it must be remembered that transferring the records is only the first step—next; it must be interpreted and used by all receiving systems.
Regulations and Interoperability Standards in Healthcare
Healthcare is a strategic sector involving many entities. As such, regulations and standardization are crucial for the efficient and secure functioning of all the contributors to the industry.
In the USA, one such regulation is the Health Insurance Portability and Accountability Act (HIPAA). It has revolutionized healthcare data protection in the country by introducing security and privacy standards for protected health information (PHI).
But as much as HIPAA focuses on privacy and security, it also recognizes the need for health data to flow through the healthcare ecosystem. For that purpose, HIPAA defines what records can be shared and how to make the transfer secure. The regulation establishes three areas where providers can share PHI without explicit patient consent: treatment, payment, and healthcare operations.
With that, physicians and health systems can freely access patient records if they’re used to treat, get payment for services, or improve operations. Other uses include consulting with other providers about treatment, sharing information as part of a claim for payment to a health plan, and health plans using PHI to provide patient service.
Thus, despite its focus on data privacy and protection, HIPAA supports interoperability by enabling providers to share PHI seamlessly required for patient care, quality improvement, and other core activities.
Similar regulations govern the use and sharing of healthcare records in other regions. In the EU, information concerning health is considered a special data category under the General Data Protection Regulation (GDPR), the EU’s main data privacy act. For healthcare-specific purposes, GDPR is extended further by the European Health Data Space—a set of rules and standards created to support patients and healthcare-oriented organizations in managing and using data.
Although GDPR applies only to EU member states and non-EU organizations that process EU resident data, it sets a standard for other countries seeking to regulate data usage and protection. Among national data policies inspired by GDPR are Brazil’s LGPD, Turkey’s LPPD, and Egypt’s DPL.
More recently, standards were developed that are concerned precisely with facilitating interoperability. Notable examples include Fast Healthcare Interoperability Resources (FHIR) created by the standards development organization Health Level 7 (HL7) or Trusted Exchange Framework and Common Agreement (TEFCA).
Their main goal is to reduce the gap between disparate healthcare IT systems and enable their unification. This is done by:
- encouraging the use of common data exchange technologies like REST API,
- adopting standards and concepts familiar to software developers like XML, JSON, HTTP, and OAuth,
- prioritizing ease of use and implementation,
- basing development on widely available resources and tools,
- focusing on modern security standards.
These standards aim to make interoperability easier to adopt and enable faster and simpler application creation. The need for standardization was recognized by WHO, which recently announced plans to cooperate with HL7 on its global health interoperability strategy.
Achieve Full Interoperability in Healthcare with RPA Automation
Although standards and regulations offer crucial support for connecting EHR systems, dealing with large volumes of data remains challenging. Healthcare organizations are increasingly adopting automation technologies such as Robotic Process Automation (RPA) to facilitate EHR operations.
The primary use of RPA in interoperability is to facilitate data transfer through EHR automation. Accessing and moving records requires healthcare staff to log into and out of multiple applications and copy-paste patient records between them. This manual workflow is inefficient and prone to errors and inconsistencies in critical datasets.
RPA healthcare solutions may automatically extract and exchange patient data between disparate EMR/EHR platforms, billing systems, physician dashboards, and other programs. With that, providers save time and combine all data into a single ecosystem. Centralizing data prevents patient records from ending up in silos within healthcare organizations, reducing the cost and effort necessary to retrieve and move them between entities. All that without errors or records getting lost along the way.
DocPlanner: Faster Patient Profile Creation

To illustrate that, let’s look at the story of DocPlanner. The leading medical scheduling platform turned to us to automate the integration between their system and EHRs/EMRs used by providers. With RPA EHR automation, DocPlanner could expedite patient profile creation and move all necessary data from their partners’ systems. From there, we’ve gradually added multiple additional features, such as automated data migration between all connected apps or visit rescheduling and cancellation.
Most importantly, readily available patient data opens up further healthcare process automation opportunities. RPA developers can support healthcare providers in:
- medical billing and coding,
- claims processing,
- appointment scheduling,
- data migration,
- placing lab and medical supply orders,
- customer service,
- invoicing,
and many more mundane, data-based healthcare workflows.
Pain Treatment Centers of America: Streamlined Claim Submission
Another case from our portfolio demonstrates how a single automation project can become an ongoing, organization-wide improvement process. Our collaboration with the Pain Treatment Centers of America practice network started with a simple task: automating the claim submission process. Encouraged by the successful deployment, our customer decided to scale up their automation. As a result, we created dozens of purpose-made bots that handle a range of healthcare processes across the network, from payment eligibility checks to write-offs and data retrieval.

Interoperability through Automation
From clinics to insurers, connecting all entities involved in the treatment process is crucial for a positive patient outcome. The better the interoperability, the faster and more reliable that process becomes—and with RPA, you can bring all your systems closer together through efficient data processes.
Want to find out more about automation and healthcare interoperability? Get in touch! Or, check out our automation ROI calculator to assess the expected return on RPA investment in your organization.









.png)



