Claims Management Automation
Faster claim processing – from charge entry to clearinghouse acceptance. Fits every EHR – no matter how complicated your processes are.

Integrates with my system? Yes, Epic, Meditech & more.
Setup time? Weeks, not months.
Secure? 100%. HIPAA-compliant, fully encrypted.
No more breaks in cashflow.
Manual work only drives A/R days up
Missing clearinghouse acknowledgements, stalled batches, payer rejections, and unreturned statuses - even one missed update pushes claims into aging and slows your cash flow.
Spreadsheets won’t scale. Claims volume will.
Agentic AI speeds up entire turnaround
Clearinghouse reconciliation, payer responses, adjudications - our AI Agent delivers real-time visibility across the entire claim lifecycle.
It automatically flags what’s stuck, follows up on what’s missing, and routes only true exceptions to your team.
How Claims Management Automation Works
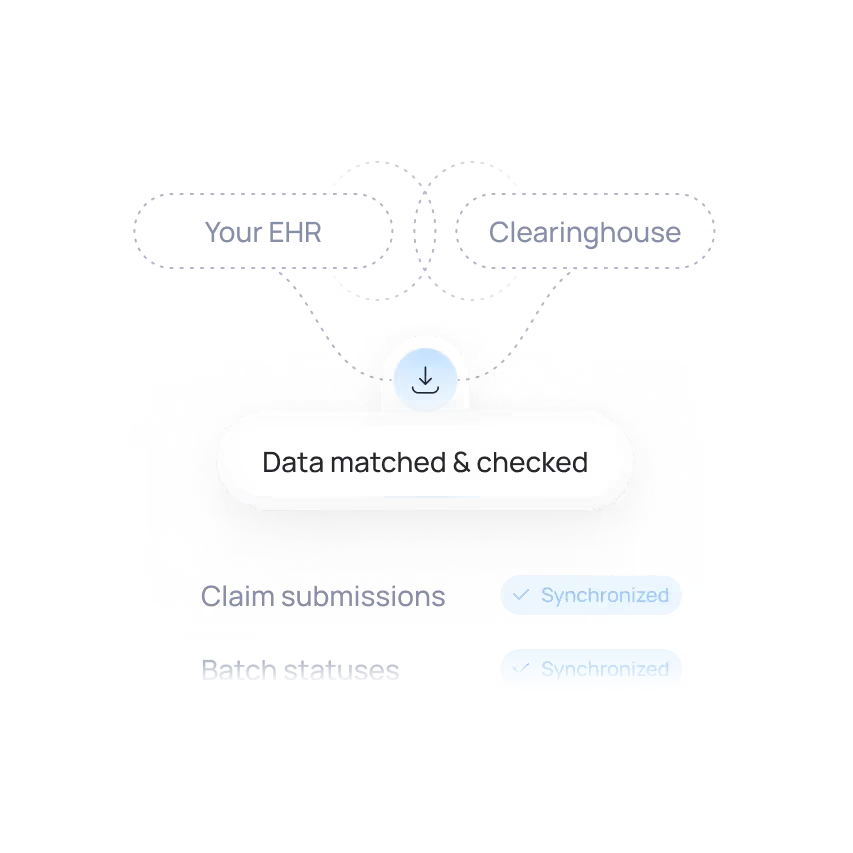
Data Cross-check
Syncs with your EHR and clearinghouse to pull claim submissions, batch statuses, and acknowledgements.
All data. In real-time. At your disposal.
Clearinghouse & Payer Tracking
Monitors clearinghouse acceptance, payer acknowledgements, stalled batches, and missing statuses in real time.
No more missed updates. No more being left hanging.
Adjudication Monitoring
Tracks payer review, detects rejections or delays, and alerts your team the moment a claim needs action – before it slips into aging.
No more delays. No more system hopping. No more waiting.
Ready to automate your claim management workflow?
Karl – our CTO loves to discuss the ROI. Feel free to book a call with him.
In just 15 minutes, we’ll cut through the noise and see if automation works for you.

Results you can expect.
Proof that speed = cash flow.


98% Reduction in Manual Claim Prep | Claims Management Automation
Gentem’s case demonstrates how an agentic AI automation layer strengthens the entire claims lifecycle without adding headcount or forcing changes to existing EHRs with 1,2 FTE saved a month
98%
Reduction in manual claim prep. See how an automated EHR-to-claim data pipeline removed up to 250 hours per week of manual RCM work.


70% Faster Claim Turnaround Time (CTT) | Claim Management Automation
SuperBill’s case shows the power of document-to-claim automation. Our prior authorization AI agent made Claim Turnaround Time (CTT) by ~70%
70%
Faster Claim Turnaround Time (CTT). See how document-to-claim automation accelerated out-of-network reimbursement workflows.

They were easy to get in contact with and the whole collaboration went smoothly. The automation has saved us a considerable amount of time. Everyone in the team confirmed it works fantastically and that it’s freed them up a lot of time.

Thanks to Flobotics, we have increased our sales conversion rate by 3%. The team communicates effectively and is proactive both in the product discovery and development stages. I love the business drive of the team as well as their flexibility and readiness to address all the needs.

Our work with Flobotics helps facilitate the process. It leverages the capabilities of different systems, to make it happen, as no individual system has the capability on its own.We’re very satisfied with their work.

Wait, there is more?
Yes! We also specialize in remaining RCM processes.

Denials Management Automation
Hunts and classifies denials early to stop them from aging out.

Prior Authorization Automation
Automate your PA process. No API required.

Eligibility Check Automation
24/7 patient coverage verification - all without human supervision






.png)