Claude for Healthcare
Anthropic built the FHIR and prior auth skills. Your full patient record, payer policy, and prior auth packet processed in one pass, configured to your organization's policies.
Claude will unlock your capacity -> let us implement it.

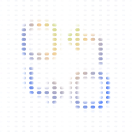
Prior authorization, ICD-10, CPT.
Full HIPAA compliance.
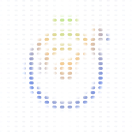
Epic, Cerner, HL7, FHIR.
No API needed, no replatforming.
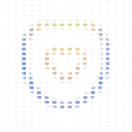
You gain a vetted automation partner
We focus on 100% ROI.
Every Process.
Every System.
Prior Auth Automation
Built on HIPAA-ready infrastructure with safety guardrails designed for healthcare. Claude validates provider NPI via NPI Registry, checks CPT and ICD-10 codes, pulls coverage requirements from the CMS Coverage Database, and cross-references clinical criteria against patient records — tracing every answer back to its source so you verify before you approve. Work that took hours of manual cross-referencing, done in seconds.

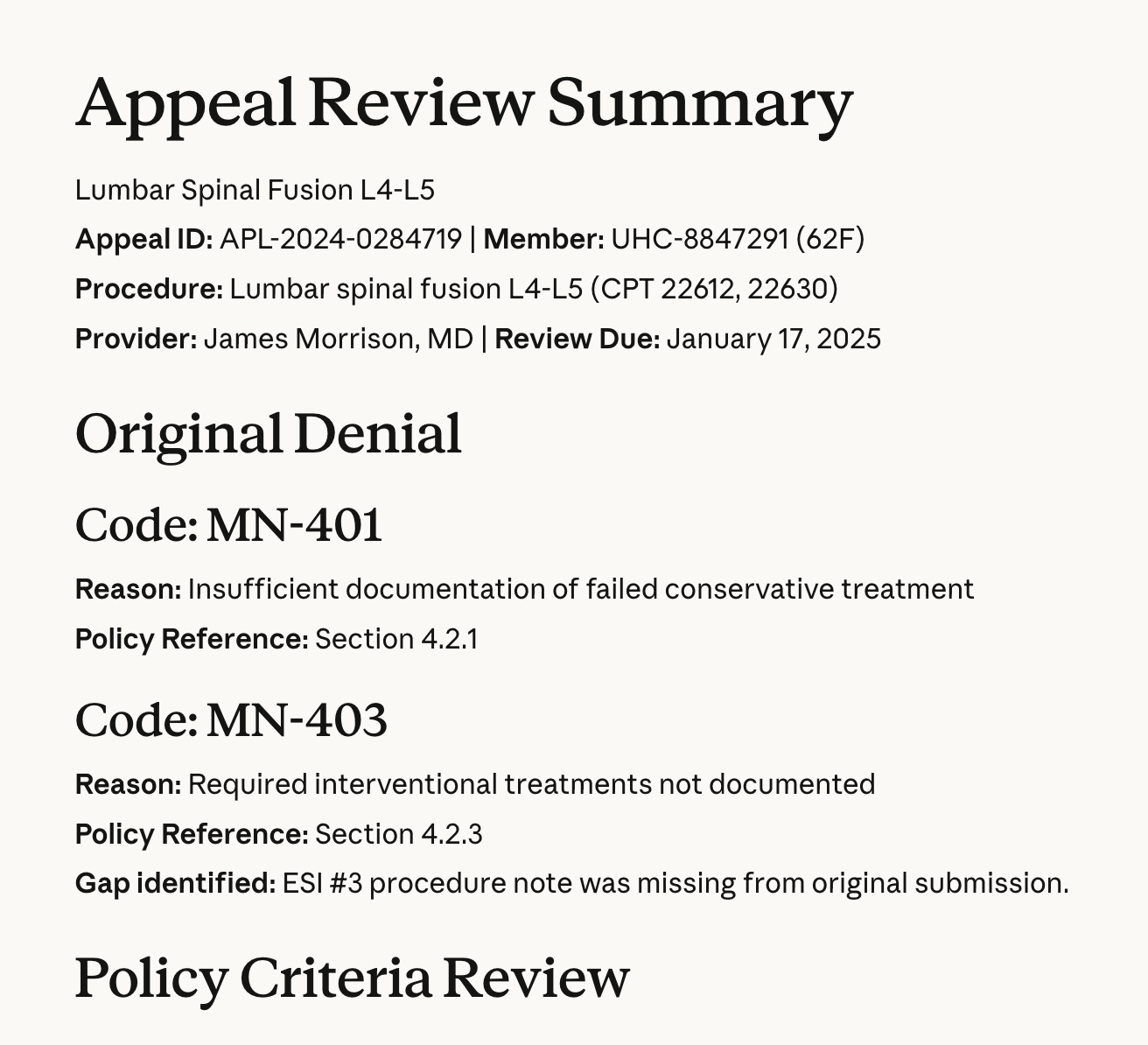
Insurance Claims Appeals
Claude understands the complexity of payer rules, medical necessity criteria, and coverage policy. It reviews your denial reasons, cross-references clinical records against policy requirements, identifies every documentation gap, and drafts a comprehensive appeal with source-cited clinical evidence for each denial code. Answers traced back to the source — so your team reviews decisions, not disasters.
Care Coordination & Triage
Connected to Function Health, HealthEx, Apple Health, and Android Health Connect — Claude reviews patient portal messages with full health record context, flags urgent clinical issues for immediate attention, drafts responses to routine questions, and routes billing, referral, and scheduling messages to the right team. Safety guardrails ensure clinical issues are never triaged down when they should escalate up.

Ambient Scribing
Claude understands the complexity of medical coding and clinical decisions. From a visit recording, it generates the full visit summary, HPI, physical exam, ICD-10 assessment, and care plan — cross-referenced against PubMed clinical guidelines and the patient’s chart. Flags medication sensitivities, E/M level mismatches, and billing gaps before anything reaches the chart. 47 seconds from a 12-minute recording.

ICD-10, CPT & HCC Coding
Claude connects directly to CMS Coverage Database, ICD-10, NPI Registry, and PubMed — reviewing every code against clinical records, payer rules, and coverage policy before submission. It shows you where every answer came from so your coders can verify, not guess. Work that took days now takes minutes. Fewer errors entering the pipeline means fewer denials coming back.

agentic AI automation is a natural step in RCM evolution.
And we have several proof of this.


+$50K Saved in 1 Month | AI Agent For Denials Management
This case demonstrates how AI-driven denial automation eliminated ~90% of manual rework, reduced claim processing time from ~6 minutes to ~30 seconds, cleared 80% of a 3,000-record backlog in three weeks, and delivered $90K+ in savings with 500+ hours saved monthly.
+$50K
Saved in 1 Month. Discover AI automations that reduce 90% of manual re-work for RCM teams.


70% Faster Claim Turnaround Time (CTT) | Claim Management Automation
SuperBill’s case shows the power of document-to-claim automation. Our prior authorization AI agent made Claim Turnaround Time (CTT) by ~70%
70%
Faster Claim Turnaround Time (CTT). See how document-to-claim automation accelerated out-of-network reimbursement workflows.


98% Reduction in Manual Claim Prep | Claims Management Automation
Gentem’s case demonstrates how an agentic AI automation layer strengthens the entire claims lifecycle without adding headcount or forcing changes to existing EHRs with 1,2 FTE saved a month
98%
Reduction in manual claim prep. See how an automated EHR-to-claim data pipeline removed up to 250 hours per week of manual RCM work.
Ready to automate your business processes?
Karl – our CTO loves to discuss the ROI. Feel free to book a call with him.
In just 15 minutes, we’ll help you assess whether automation is right for you.


I admire their ability to meet and exceed our requirements and expectations.

Thanks to Flobotics, we have increased our sales conversion rate by 3%. The team communicates effectively and is proactive both in the product discovery and development stages. I love the business drive of the team as well as their flexibility and readiness to address all the needs.

I am thrilled with the collaboration so far and looking forward to expanding it in the future!

Wait, there is more?
Already in healthcare? We go deeper — end-to-end RCM automation is our core.

Denials Management Automation
Hunts and classifies denials early to stop them from aging out.

Claims Management Automation
Tracks claims and flags denials before they cost you.

Prior Authorization Automation
Automate your PA process. No API required.

Eligibility Check Automation
24/7 patient coverage verification - all without human supervision





.png)
.png)